The missing piece about why your knee hurts going up stairs
Many of my clients with knee pain tell me that their pain or popping sensation either comes on or gets worse when going up and down the stairs.
Let me break down why this happens and sort through common myths and what actually helps; especially if you’ve been wondering why your knee pain isn’t improving despite doing “all the right things”
The gap in most knee pain explanations
Most explanations for knee pain talk about what is happening in your knee, not why it’s happening.
You might have been told things like:
your kneecap isn’t tracking right
your scan shows arthritis
you have a meniscus tear
or your muscles are out of balance (like weak quads or tight hamstrings or IT band etc)
These explanations describe what your knee is going through. They don’t explain what your body is doing that’s causing it. This is especially confusing when the pain shows up on just one side, like in cases of right knee pain that seems to come out of nowhere.
Even in medical research on things like patellofemoral pain syndrome, the focus is shifting. It’s less about just the knee itself, and more about how your whole body moves and how pressure goes through the joint.
Still, the usual advice is to strengthen certain muscles, stretch others, or change your diet.
Before we talk about the extent that those things help, let’s first look at what your body actually needs to do to keep your knees comfortable and pain-free when climbing stairs.
The physics of happy knees
For your knees to feel good going up stairs, your whole body has to work together.
It’s not just about the knee.
Here are a few things that matter:
How well your standing leg supports you, so the other leg can step up easily
How your foot and ankle lands on the step
Whether your knee stays lined up over your foot
What your upper body (head, chest, and spine) are doing to move your weight towards the leg you’re stepping onto
Why your knee might feel fine walking but climbing stairs hurts
Climbing stairs is a lot like walking but stairs add an extra challenge. You’re not just moving forward.
You’re also lifting your whole body up and over your leg with each step.
That extra “up” part means your body has to work together better than it does on flat ground.
If it doesn’t, your knee ends up doing more of the work.
That’s why your knee might hurt on stairs, even if walking feels totally fine.
Situations where strengthening doesn’t help
Two people can have the same diagnosis, the same strength levels, and even the same scan results and one goes up stairs comfortably while the other has pain. This is because strengthening muscles doesn’t necessarily change how you move. If your body hasn’t yet figured out a better way to move as a whole, the vulnerability in the knee persists.
What I’ve seen in my practice over the last 10 years is that many people end up strengthening the wrong muscles, making the pain worse. And it’s hard to stick with the routine when you worry that exercise might make your pain worse. This can feel like a double whammy!
That’s why I focus on improving how your whole body works together.
When your ankles, legs, hips, and spine start moving in better coordination, the strain on your knee naturally goes down.
Here’s a client experience to give you a sense for what this can feel like:
“How to organize my body when climbing stairs is the single most life-changing thing I learned working with Shrutee. Earlier, I used to feel a shock-like sensation, like I was going to lose my balance. Instead of avoiding the stairs, on busy days I now use going up and down stairs to get my practice in and it feels great!”
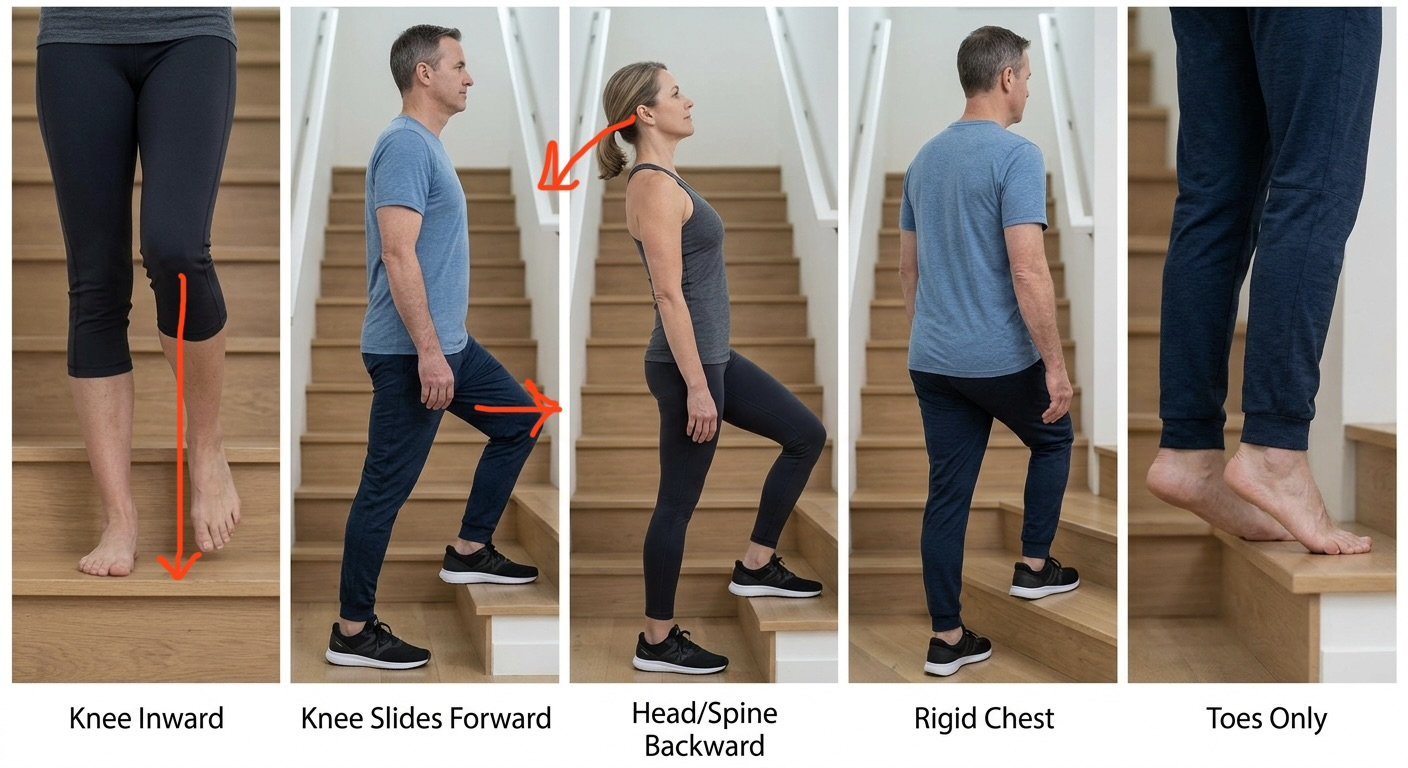
5 common mistakes causing knee pain climbing stairs
Here are some common mistakes I’ve seen people make over and over again. The 1st and 5th mistake are pretty easy to spot and for those of you that are self-starters, I urge you to start observing those in yourself right now.
1. The knee drifts inward instead of being stacked over the foot
This is by far the most common and relatively easy to observe in yourself. The knee ends up slightly inside the foot rather than stacked over it, referred to as dynamic valgus or medial knee collapse in medical language. When that happens, your knee twists while you’re trying to push upward. While the knee joint has some twisting ability to accommodate for walking on uneven ground, it wasn’t meant for constantly walking like this. It’s like putting weight on an unstable foundation and those small micro stresses to the soft tissue in your knee do add up over time.
2. The knee slides forward ahead of the rest of your torso
Also referred to as “Quad dominant” reaching, Here the knee slides forward ahead of the foot, and the rest of the torso. It’s as if the knee is trying to arrive at the next step before the rest of your body. This places the joint in a high-shear position before your weight has fully shifted onto the supporting leg.
3. Leaning back or posterior weight shifting
Many people subtly throw their head and spine backward as they step up. This forces the leg to pull the body weight upward rather than receiving it. This creates unnecessary tension in the patellar tendon. This is often seen in people that tend to overcorrect their posture.
4. Rigid spine
Your body naturally needs to turn slightly toward the stepping leg to facilitate a clean weight transfer. When the chest and ribs stay rigid, you never fully "arrive" on the stepping leg, leaving the knee to compensate for the lack of spinal rotation. This is often the result of poor communication between upper and lower body.
5. You tiptoe up the stairs instead of landing on the whole foot
Some people hurry up stairs on their toes without letting the heel come down at each step. This is also called ‘forefoot landing’ and can result in tight calves and hamstrings over time. Without the heel helping to support your weight, the knee often picks up the extra load, which can make stairs feel uncomfortable or painful over time.
Many of these patterns are hidden in plain sight. I hope that you got a chance to observe at least one in yourself now.
Taking pauses through your day, bringing your awareness to these habits is the first step in recognizing the importance of your whole body movement in the health of your knee. The next step is to invite your nervous system to begin changing these with a structured somatic practice.
Ready to start changing these in a reliable and systematic manner? This is exactly why I created the Smart Relief Guide on ‘3 Hidden Mistakes that make your Knee Pain worse” and what to do instead.
Inside, you’ll discover:
why your knee pain may not actually be a knee problem
how certain “good” habits can keep you stuck in the same pattern
simple ways to begin shifting how your body organizes movement without forcing or overcorrecting
Frequently Asked Questions
If my MRI shows arthritis, can movement habits really change the pain?
Yes. Research has shown that the correlation between "wear and tear" seen on imaging and the actual experience of pain is surprisingly low. A study published in the British Journal of Sports Medicine found that many people with no pain at all show signs of arthritis on scans. Pain is often more about how you load the joint than the structural state of the joint itself.
Is "crepitus" (that popping sound) dangerous?
Not necessarily dangerous in an instantaneous way. But its indicative of inefficient co-ordination and resulting slow decline in the health of your knees.